If you are interested in a personal coaching session for stroke recovery, which would include teaching you or a caregiver acupressure and therapeutic exercises you can do to speed healing, you can schedule a telehealth appointment here! Please note I am in the Pacific time zone.
EDIT 1/22/15: Since I posted this I’ve gotten a lot of emails from people all over the world wanting to know if I can help them. Unfortunately, I don’t know anyone I can refer you to outside the US… outside the American Pacific Northwest I do not have much connection with other acupuncturists.
It’s impossible for me to know how many sessions your recovery would take. There are so many factors – your condition, your general vitality, your diet, how much physical therapy you do, etc.
To find a local acupuncturist, first ask around and read a lot of reviews (Yelp, Google, even ask your neuro docs if they know of someone local). There’s a big variation in skill / talent among practitioners, and there are lots of different styles. Feel free to try a few and fire anyone who doesn’t mesh with you. Be aware that with neurological repair it may take weeks to get observable results, which can complicate your decision. Be patient.
If you can find someone locally who does medical massage (advanced techniques are much better for this than regular relaxing massage or “deep tissue”), that will be helpful. Usually the muscles and nervous system need to be re-trained so they aren’t so spastic.
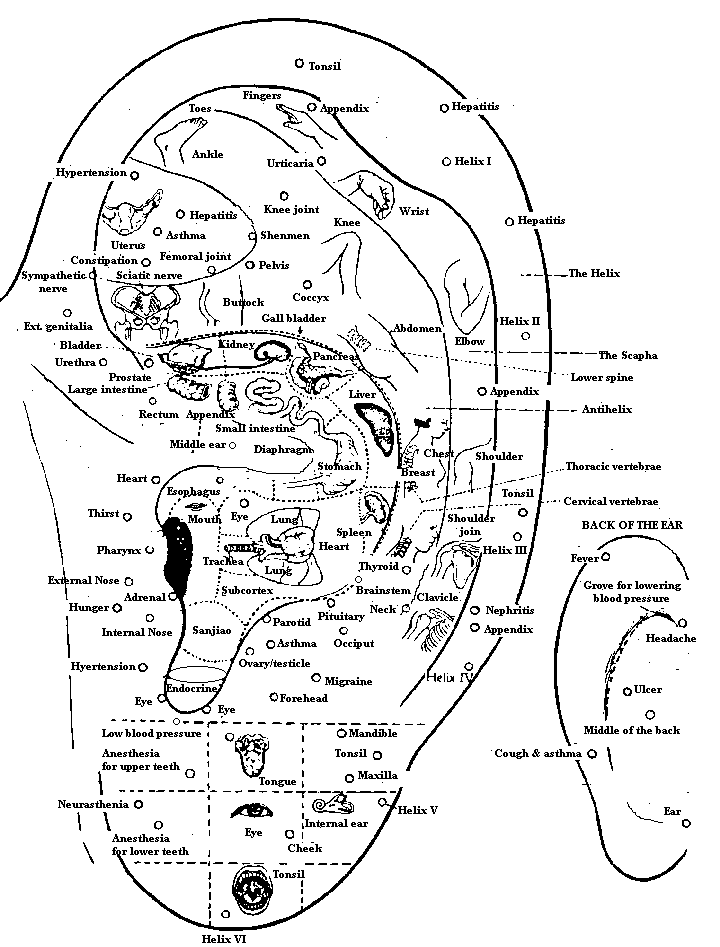
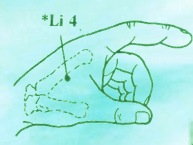
I recommend self-stimulation (rub with fingertips) all over the ears and scalp, especially Du-20 and the scalp from the ears forward. Also, stimulate points LI-4, LV-3, and GB34, and BL 62 (just under the outside ankle bone). You can do that up to a few times a day.
Use regular (2-3 times a day) exercises to try move your body – even if you can’t see it move – imagine it and try. Visualize doing a movement you know well, like a sport, playing a musical instrument, or typing. Moving – especially novel movements – will help your neural repair more than anything else. It’s ok if you are shaky or inaccurate in your motor control, you just have to keep trying things.
Avoid processed food. Good fats (avocado, nuts, seeds, fish, coconut oil, extra virgin olive oil, etc) are essential to support nerve repair. Eat lots of veggies, cooked so you get more nutrients out of them, and good quality protein (grass-fed / pastured animals).
Most important – try to keep a positive outlook. I know it’s very difficult in a frustrating situation, but focusing on the good parts of your life will keep your body less stressed, and it will heal better (When you are in “fight or flight” mode your body won’t expend energy on healing / digesting as much). Meditation, breathing exercises, etc can be helpful.
If you are doing this research on behalf of a loved one, I would also recommend you look into a caretaker support group for YOU. It can be a huge stressor. In addition to practical advice, you can really benefit from talking to someone who understands your situation.
I hope this helps you in your recovery. If I can be of further help please let me know!
*****************************
EDIT 7/1/13: A note on longer-term neurological repair: The current “common knowledge” in the Western medical world is that most nerve repair will happen within 6 months of the injury. After that, they say, you are stuck with whatever impairments you still have. I want people to know that while it’s harder to achieve progress past the 6 month mark, it’s by no means impossible! I had a patient who suffered a stroke 17 months before I saw her. When we met, she was locked into position in bed, bent, twisted and looking into the corner of the ceiling. She was unable to move her limbs or speak. When I arrived for her fourth visit in as many weeks, she was sitting up and cracking jokes. Her legs had straightened out, and she had regained enough control of her hands to eagerly anticipate knitting again! While these results are not average, they provide hope, as does this article.
NOTE: This is a transcript of a presentation geared to healthcare providers who have no experience with Chinese medicine (doctor’s office staff, etc), and focuses on recovery rather than prevention. It was written as part of my thesis project for my Master’s Degree at the Oregon College of Oriental Medicine in 2005. It was updated with the newest demographic information in 2011 but otherwise left in its original form.
I’ve always had a personal love of the science of the human body. I was a bodybuilder and personal trainer focusing on rehabilitation and core strength for three years. Working with my clients was thrilling but I knew I needed more education. I took the full battery of medical prerequisites and went to chiropractic school. After the first year I knew their method of adjusting wasn’t a good fit for me, but I’m grateful for what I learned in the cadaver lab and in lecture classes. I took that base of knowledge to the Oregon College of Oriental Medicine where I earned a Master’s degree in Acupuncture.
According to the American Stroke Association, nearly 800,000 people each year suffer a stroke in this country (this number was 700,000 in 2004). On average, an American suffers a fatal stroke every 3-4 minutes. It’s the third-largest cause of death behind heart disease and cancer. Strokes are not always fatal, of course. They are a major cause of disability, and are responsible for an estimated 550,000 disability cases per year. For many survivors, the ordeal may be just beginning.
More than 75% of stroke patients have motor impairments, often resulting in disability, such as impaired ambulation and inability to perform activities of daily living (ADLs) (Wojner). ADLs are the basic tasks of everyday life such as eating, bathing, dressing, toileting, and transferring (Wiener). Suddenly being handicapped can cause embarrassment, frustration, and profound depression for the post-stroke patient. Caretakers and family members also experience stress, both psychological and financial. Americans will pay about $68.9 billion in 2009 (this number was $57 billion in 2005) for stroke-related medical costs and disability (American Stroke Association).
CVAs – Cerebral Vascular Accidents – come in two flavors, ischemic and hemorrhagic. The ischemic (lack of blood) type is much more common (82%) and results from a clot stopping blood flow to part of the brain. It could be a local cerebral thrombus, or an embolism from a distant clot that occluded a cerebral artery. The hemorrhagic type, as its name suggests, results from bleeding from an intracerebral artery. In either case, the patient can suffer long-term ill effects ranging from poor memory or speech problems to paralysis.
TIAs – Transient Ischemic Attacks – are mild or “mini-strokes.” They produce brief periods of damage that resolve without medical intervention, sometimes within minutes.
Unfortunately, with most CVAs there are lasting repercussions. Symptoms will vary with the location of the brain damage. If Broca’s Area is deprived of oxygen, for example, the patient will have difficulty with speech production. If the posterior brain is affected, the patient will have impaired vision. Today I will focus on treating damage of the motor area of the brain.
After recovery from a stroke, a patient can frequently have motor weakness on one or both sides of the body. Further impairing mobility and function in this patient population is spastic hypertonia. This abnormally excessive muscle tone can cause many problems, including pain, loss of free movement of a limb, and interference with the ability to walk and perform daily activities, such as bathing or dressing. It also may cause the limb to become “fixed” or frozen in an uncomfortable position (Meythaler).
There are two nerve cells that control each muscular contraction, the upper and lower motor neurons (UMN and LMN). The upper motor neuron begins in the brain and descends through the spinal cord. It synapses (meets) with the lower neuron, which goes to a muscle. The LMN creates contraction, so damage below the synapse will result in flaccid paralysis. This is the typical post-trauma paraplegic with atrophied legs. By contrast, the upper motor neuron normally inhibits contraction. When the UMN is damaged in a stroke, the muscles are never turned off: patients have perpetually spastic muscle tone. They might have their arms pulled up tight against their bodies, or legs that want to stay crossed. In cases that affect fine motor control, writing and other small tasks are compromised. You may see a similar pattern in people who have suffered head trauma. Post-stroke spasticity creates uncontrollable muscle tightness that can cause painful muscle cramps, particularly in the arm and leg.
The current allopathic toolbag for hypertonicity is quite large and still evolving. Systemic antispasticity drugs have fallen out of favor, because they are nonselective in action and may cause functional loss of normal muscles. Some doctors like to use muscle relaxants, like tolperisone – a centrally acting muscle relaxant with membrane stabilizing activity. Stamenova conducted studies that showed tolperisone to be safe and effective in reducing spasticity as measured by the Ashworth scale.
The most common type of treatment is a local blocking agent: a medication that will deliberately impair the transmission between lower motor nerves and muscles. When the nervous system sends these abnormal commands to contract, the messages are no longer transmitted to the muscle and the muscle remains relaxed (Bakheit). Botulinum toxin has been widely used with good effects and can be performed as an outpatient procedure without anesthesia.
The pharmaceutical management of spastic hypertonia following stroke has generally been confined to the use of approaches that reduce activity at the neuromuscular junction (botulinum toxin), inhibit the release of calcium from the sarcoplasmic reticulum (dantrolene sodium), or those that act centrally (baclofen, diazepam, and clonidine). Ablative procedures are performed, such as phenol injections to the motor points or nerve blocks by injection. These procedures generally require repetition and have been associated with permanent weakness, and loss of muscular control (Meythaler).
Most recently, intrathecally delivered baclofen has been established as a treatment method in acquired brain injury. A catheter is inserted into the spinal canal and a radio-transmitting device delivers medication directly into the fluids surrounding the spinal cord. Baclofen binds to presynaptic GABA-B receptors within the brain stem and other central nervous system (CNS) sites. By blocking the transmission of neural messages, it prevents muscular contraction.
Physical therapy is another commonly prescribed modality for stroke survivors. This can range from gait retraining with a parachute harness over a treadmill, to personal training with free weights or elastic bands. Occupational therapists can intervene with training of sensory-motor functions, training of cognitive functions, training of skills such as dressing, cooking a meal, or performing domestic activities, advice and instruction in the use of assistive devices, provision of splints and slings, and education of family and primary caregivers (Steultjens). Previously, doctors feared that physical exercise would exacerbate spasticity. Research has shown instead that exercise such as pedaling a bike is a beneficial intervention for achieving gains in muscular force output without worsening motor control (Brown).
Now that we have an overview of the main techniques used to treat spasticity, let’s compare their outcomes and side effects:
There are a number of studies on botox injections as an antispasmodic, with both upper and lower limbs. Success rates in reducing spasticity are impressive, but are accompanied by muscle weakness. For example, Berlin’s Dr. Hesse noted weakness in the anterior tibialis (shin muscle, which lifts the foot) after injections of the gastrocnemius calf muscle. Side effects are known to include bleeding, skin rashes, or tenderness at the injection site, as well as flu-like symptoms (Bakheit, et al). The main drawback to botox injections is the short-lived benefit: Three months of relief seems to be average (Bakheit, et al).
Unlike other drugs used to treat spasticity, tizanidine has not been shown to cause muscular weakness (Wallace). However, it has other significant drawbacks. The side effects seen with tizanidine in this study were similar to those previously reported. In both Wallace’s and Gelber’s work, the most common were sedation, dizziness, dry mouth, and hypotension. Nearly 15% of their patients withdrew from the study because of these side effects. All of these patients developed these side effects at very low doses of tizanidine.
Intrathecal Baclofen delivered by a pump can vary the amount of medication during the course of a day. It’s effective for the lower limbs and torso, but has less predictable effects for upper limbs. Intrathecal delivery causes less sedation, lethargy, and weakness than oral Baclofen, with a stronger nerve action. It requires that a surgeon or an anesthesiologist implant a small tube into the spinal cord and a pump under the abdomen skin, and is best used for patients that have severe spasticity, particularly those with a spinal cord injury or multiple sclerosis (Ivanhoe).
Although all of these types of therapies have provided relief for patients, there is still a need for alternative therapy. Acupuncture is an appropriate adjunctive therapy for those patients who want to avoid additional drugs. Many of the patients who suffer strokes tend to be taking multiple medications. Providing relief without inducing additional drug interactions is a beautiful bonus.
Acupuncture also provides a more holistic answer when compared to botox injections. Why deaden an operating nerve (the lower motor neuron) when the damaged UMN is the problem? Two wrongs do not make a right – they create further insult to the body. TCM (Traditional Chinese Medicine) focuses on healing the original injury. Needles have been used with good success in treating neurological problems and can help stimulate nerve regrowth and recovery.
There are many styles of acupuncture, including Japanese, 5 Elements, Classical, etc. but this lecture will limit itself to TCM acupuncture. Its roots are ancient: some sources indicate needles were used for healing as much as 4000 years ago. Acupuncture in its present form was practiced 2000 years ago. Much of the theory is based on empirical science – that is, trial and error! Over 40 centuries they figured out some pretty amazing things about the human body. Before I can explain them, though, it’ll be helpful to understand the framework of TCM theory.
Acupuncture deals primarily with Qi, usually translated as Energy. There are many types of Qi. Some represent functions as well as energy. For example, our Defensive Qi, (Zheng Qi) does battle with pathogens (Xie Qi). Our Prenatal Qi (affected by genetics and the prenatal environment) is sort of our potential vitality (Jing). Children with birth defects are said to be deficient in Prenatal Qi. Postnatal Qi is affected by diet and life experiences, and we can use it to supplement and fortify our vitality. Too much stress or a poor lifestyle will drain our Jing and lead to premature aging.
The most basic differentiation in Chinese Medicine is that of Yin and Yang. Yin is the darker, moister, interior, still, nourishing, more feminine half. Yang is light, dry, exterior, expanding, moving, and more masculine. As applied to anatomy, the front and lower parts of the body are Yin. The back and upper body are considered more Yang. On the lower limbs, medial is Yin (think interior) and the lateral aspects are Yang. This will be important later when we devise a treatment strategy.
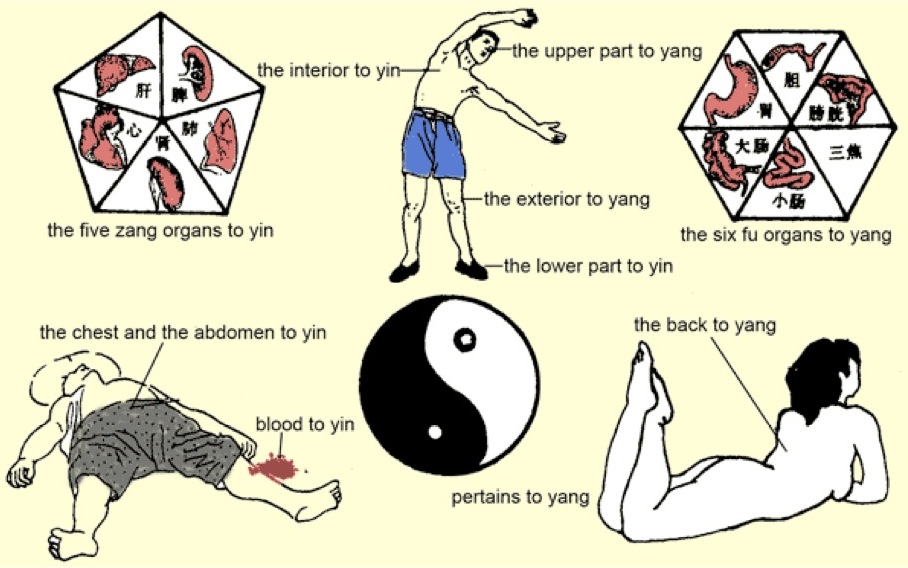
Yin & Yang aspects of the body
Our Qi flows in a series of meridians, or channels. These are rivers of energy flow that travel along specific paths, and were mapped out 2000 years ago. Chinese anatomical position describes the arms as lifted straight up, so the body forms a symmetrical X. The Yang channels start high and travel downward: from fingertips to the head, and head to the toes. The Yin channels start below and rise, to carry nourishing energy upwards: they run from the toes up, and from the torso to the fingertips.
At some areas of the body, the Qi bubbles closer to the surface. In these places we can access the energy more easily. These are acupuncture points. Acupressure, simply pressing with a fingertip, is also effective at these spots. There are 365 points on the channels. Including auricular sites and extrachannel points, there are about 1000 altogether.
The 12 ordinary meridians are each linked with an energetic organ. These are the Heart, Pericardium, San Jiao, Small Intestine, Large Intestine, Lung, Kidney, Bladder, Liver, Gallbladder, Spleen, and Stomach. The organs are bundled into Yin/Yang pairs. The eight extraordinary meridians are not linked to organs. Instead, they treat on a more constitutional level. We’ll see later how these eight can be particularly useful in treating post-stroke spasticity.
The Chinese have ascribed energetic properties to the various organs. Each organ is tied to one of the five elements: Wood, Fire, Earth, Metal, and Water. The elements are associated in a complex series of cycles, so each can influence the others. The organs (and elements) are also linked to a sense, flavor, color, season, and emotion in addition to their physiological function. Some of these make obvious sense in terms of medical science, like the Heart being the master of Blood.
Other organs may seem stranger at first glance. The Liver, for example, is in charge of emotions and smooth Qi flow. Constant circulation of energy through the meridians is considered essential for health. When Liver dysfunction prevents proper energy flow, the condition is called Liver Qi Stagnation. Anger or irritation is a common side effect. This organ is linked with female reproductive health. If you think about a woman suffering from PMS, you can see that her Liver Qi isn’t moving effectively. Stagnation causes cramps, and her mood swings are legendary. This syncs with modern science if you think about the biological liver’s role in metabolizing estrogen and other hormones.
The liver’s partner is the Gallbladder. Interestingly, it is associated with decision-making and fear vs. boldness. Herein may lie the root of the phrase “Why, the GALL of that man!”
The San Jiao is analogous to the lymphatic system. It controls water and fluids throughout the body, and is important to immune function. It’s paired with the Pericardium, which protects the Heart, and controls chest and abdomen issues.
The Spleen is responsible for transforming energy from food into energy for the body, so it takes on the functions of the biological pancreas and small intestine. If the Spleen is not functioning well, it will produce Phlegm. This can be visible Phlegm – nasal discharge or coughing with sputum – or Invisible Phlegm, which manifests as mental illness or interference with cognitive processes. The Spleen’s partner is the Stomach, which is not substantially different from modern understanding of the stomach.
The Lung captures Qi from the air and is responsible for the skin system and border immunity. Its pair is the Large Intestine, which is most often used to clear heat from infection, to treat the face (where the channel ends), and to aid Qi movement in the upper body.
The Kidneys are considered the storehouse of our vitality (Jing). Our Kidney Qi declines as we age. Women in menopause are showing signs of Kidney Yin deficiency (hot flashes, vaginal dryness, etc.) while men exhibit Kidney Yang deficiency (impotence and urinary difficulties). The Bladder channel runs down the back and contains a series of points called the Shu points that address each of the organs.
Now that we have a simplified understanding of the Chinese organs, let’s examine how their dysfunction contributes to pathology. All CVAs are considered Wind-Strokes. There are four main differentiations for stroke: Liver Wind, Phlegm Fire, Blood Stasis, and Wind in the Channels.
The Liver is the Wood element. Inadequate rest, excess sexual activity, or emotional stress beleaguers Liver’s cooling Yin. When this happens, it cannot balance the Liver Yang. Now the Wood is “on fire”. Liver Yang energy will rise to the head and cause Wind, much like heat from a campfire causes an updraft. Many Chinese medical concepts are taken from observation of nature and the elements.
If a patient has worked too hard or maintained an irregular diet, the Spleen will suffer. Phlegm-Fire will congeal to cloud the brain, prevent speech, and numb the limbs.
If the Kidneys are overstressed, due to lack of rest or excessive sexual activity, they cannot nourish Marrow, which in turn cannot produce Blood. Much like a dried up river, a body with deficiency of Blood becomes a body with Blood stasis. This leads to stiffness and pain in the limbs.
A more generalized understanding of physical overwork and inadequate rest indicates weakness of all the channels. A lack of defenses means that external Wind (including environmental and microbial challenges) will penetrate and develop into internal Wind. Paralysis is a common result.
Strokes that affect consciousness or even create coma are considered to have attacked the organs (viscera) and channels, and are categorized as severe. A CVA that infiltrates only the channels (a mild Wind-stroke) will result only in unilateral paralysis, numbness, and slurred speech.
The appearance of the patient’s tongue is a valuable tool in TCM diagnostics. A purplish tongue, or distended veins on the inferior surface of the tongue, indicate blood stasis. A red tongue body indicates Fire. A stiff, deviated, or quivering tongue reveals Wind, while a sticky coating shows Phlegm. Weakness in any of the organs will show up in specific areas (Kidney at the root, Heart at the tip, etc.).
During the acute phase of the stroke, Western medical care is essential. Time lost is brain lost. TCM can’t compete with MRIs and thrombolytics, and we don’t want to! Once the patient is in a recovery phase, however, acupuncture gives excellent results in the treatment of hemiplegia and facial paralysis. Speed is key here, too. Treatment within one month is recommended. After six months, improvement will generally be slower and less substantial.
Treatment with acupuncture involves choosing points by two methods. We select points with an empirical history of treating Wind-Stroke. These include points known for Wind in general, points to aid muscular control, and points to clear stagnation and stasis. Our therapy plan should also address the channels affected by spasticity.
The eight Extraordinary channels are often used to treat deep constitutional problems. For example, Bl-62 (Master point of the Yang Qiao / Yang Moving Channel) treats muscular dysfunction impairing locomotion. This point is just inferior to the lateral malleolus. The Xi-cleft point of this same channel, ascribed with the ability to remove stagnation, is BL 59, on the lower lateral leg.

Let’s take an example of a male patient with his right forearm fixed in flexion. His arm is pressed against his side, and his hand is curled up against his chest. According to TCM diagnostics, he is afflicted with Wind in the channels. In this case, the channels affected are the Heart, Pericardium, and Lung. Each channel has a point called the Xi-cleft, which is used to dispel accumulated stagnation of Qi and Blood. These would be Lu-6, Pc-4, and Ht-6. These three points are all located on the anterior forearm. We can treat the Xi-cleft points on the affected arm, or on the opposite arm if the points are difficult to access. Wind points such as GB-20 (at the occiput), GV –20 (top of the head), GV-14 (spine, below C-7) would typically be used. LI-4 on the hand will move Qi and Blood through the upper body. St-40 on the lateral leg will disperse Phlegm.
Even within TCM, there are some differing methods of differentiation. Dr. Wu’s textbook separates “Yin Tension” from “Yang Tension” stroke, based on signs of heat or cold in the tongue and pulse. Let’s assume that our patient presents with a red tongue, slimy yellow tongue coat, and a rapid pulse. We would add LU-11, Ht-9, and PC-9. These are the points at the fingertips (extreme ends) of the affected channels.
Wong found that patients receiving electro-acupuncture left the hospital more quickly, with a significant difference in self-care and locomotion. Pei likewise found more improvement in general ADLs with acupuncture. The Swedish studies by Kjendahl found that acupuncture delivered greater improvement on a one-year follow-up.
The Gosman, Hedstrom and Johanssen studies published in Stroke found no significant differences in acupuncture vs. physical therapy in improving post- stroke ADLs, but they neglected to differentially diagnose the patients. Each received the same set of acupoints. This is a huge oversight: Specificity of treatment is essential for an effective result. Grouping everyone together is comparable to treating everyone with a runny nose with antibiotics, then concluding that medications are useless against rhinitis. Instead, we separate out the allergic, the virus-stricken, and the bacterially-infected. Chinese medicine deserves the same rigor of analysis. It’s also worth pointing out that the needles were inserted by physical therapists, not by acupuncturists. The quality of their point location and technique must be called into question.
In conclusion, post-stroke spasticity is a debilitating and frustrating hurdle for many CVA survivors. Modern Western medicine can stop nerve transmission, mute muscles, and retrain patients to help them gain control. Acupuncture can help the damaged nerves to heal, and return to normal function. If doctors and physical therapists work with acupuncturists, we can help our patients achieve a more complete recovery in a shorter period of time. Needles won’t interact with medications, so they are a great adjunct for our more elderly stroke survivors. I encourage you to reach out to Chinese practitioners and build partnerships. Ask questions. Take a look at the research I’ve quoted in my references. Refer some people, and see what happens. I look forward to working with you all!
Assessment of clinical trials
A) C. Werner, et al., Treadmill training with partial body weight support and an electromechanical gait trainer for restoration of gait in sub-acute stroke patients. Stroke, 2002; 33:2895.
1) Training: The people working with the patients were described as “physical therapists” but no additional information was given with regard to their education or experience.
2) Inclusion criteria: Non-ambulatory hemiparetic patients, 4 to 12 weeks after a first-time stroke, age less than 75, requiring firm continuous or intermittent support from at least 1 person to walk, must be able to sit unsupported at the edge of a bed and to stand for 10 seconds without assistance. Hip or knee extension deficit of less than 20 degrees, passive dorsiflexion of the ankle to a neutral position.
Exclusion criteria: Cardiac ischemia, arrhythmia, or decompensation. Resting systolic BP of 200 or more. Maximum heart rate exceeding 190 bpm minus the age of the patient. Severe impairment of cognition or communication.
3) The study was reported as randomized. Sealed envelopes were drawn to assign groups.
4) Demographics and clinical information at onset of the trial is provided and is successfully random.
5) Previous studies on post-stroke treadmill physical therapy were cited.
6) The speed and duration of the treadmill use was given in ranges only. “Physical
assistance […] was administered according to individual needs.” More detail
would be helpful in duplicating this experiment.
7) Assessment made use of the Functional Ambulatory Category (FAC), the RMA
score (gross functions and leg and trunk section), and the modified Ashworth score
testing for ankle dorsiflexion, and mean gait velocity.
8) Outcome measures were assessed by independent raters who were not involved in the therapy, and who were blind to the patient’s grouping. Interrater reliability
scores were provided.
9) Patients were aware of their grouping.
10) Six-month follow-up phone calls were placed and data was gathered on the
persistence of improvement.
B) Effects of Acupuncture Treatment on Daily Life Activities and Quality of Life A Controlled, Prospective, and Randomized Study of Acute Stroke Patients, Gosman,- Hedstrom, et al. Stroke. 1998; 29:2100-2108
1) Acupuncture was performed by 4 physiotherapists (PTs), trained together to give the same information and to use the same techniques. They were not described as having any previous acupuncture experience.
2) Inclusion criteria: Patients �40 years with an acute focal ischemic nonhemorrhagic lesion were invited to take part in the study. The stroke onset had to be less than 1 week before the randomization. Exclusion criteria: These criteria included other severe disease necessitating hospital or nursing home care; severe aphasia or unconsciousness; an earlier cerebral lesion, with a documented need of care; and treatment with a cardiac pacemaker.
3) The study was reported as randomized. Computers were used to assign groups. 4) Demographics and clinical information at onset of the trial is provided and is
successfully random.
5) No explanation was given for the points chosen.
6) The locations, stimulation, and retention of acupuncture needles were all described.
7) Assessment made use of the Barthel Index and Sunnaas Index of ADL. The NHP questionnaire, a self-instructive instrument, was given to the patient and collected on the assessment occasion by the occupational therapist.
8) Two occupational therapists (OTs), who were blinded to patient allocation after
randomization, evaluated the treatment effects on ADL, health-related quality of
life, and use of health care and social services.
9) Patients were aware of whether they received acupuncture or not. No information is available regarding the patients’ knowledge of multiple groups.
10) The assessments were performed 4 times during the first year: 3 days after
randomization and at 3 weeks, 3 months, and 12 months. The assessments were done by means of interviews and observations at the hospitals, nursing homes, and/or in the patients’ homes.
C) Acupuncture and Transcutaneous Nerve Stimulation in Stroke Rehabilitation, Barbro B. Johansson, MD, Stroke. 2001; 32: 707-713.
1) Training: “[T]he therapists received training that ensured uniformity in the treatment procedures between centers. Each therapist performed all 3 treatment modalities.” Obviously the therapists were not trained acupuncturists.
2) Inclusion criteria: Patients of all ages and both sexes were eligible if they had had an acute stroke between 5 and 10 days before randomization. Only patients with moderate or severe functional impairment at randomization were included. This was defined as a Barthel ADL Index 21 of �70 points in combination with inability to perform the Nine Hole Peg test 22 within 60 seconds (impaired fine motor function of the hand) or inability to walk 10 meters without mechanical or personal support.
Exclusion criteria: If the stroke was a recurrent one, the patient could not have been functionally impaired before the present event. Exclusion criteria were (a) previous neurological, psychiatric, or other disorder making it difficult to pursue the treatment or evaluations, (b) inability to comprehend information about the trial, (c) concurrent participation in another trial of interventions supposed to affect long-term neurological and functional outcome, and (d) failure to obtain informed consent.
3) With the use of closed envelopes and stratified by center, eligible patients were randomized in blocks.
4) At baseline, patients in each group were closely similar in all important prognostic variables. Table provided.
5) No explanation for the points chosen were given.
6) Needling technique was adequately described.
7) ADL function was assessed by the Barthel Index, 21 overall motor function by the Rivermead Mobility Index, 23 fine motor function by the Nine Hole Peg Test, 22 walking ability by the time needed to walk 10 meters (with or without mechanical support), and quality of life by the Nottingham Health Profile.
8) An independent observer unaware of the group to which the patient had been assigned performed all investigations and recordings except monitoring of adverse reactions during treatment. Patients and observers were instructed not to discuss the treatment sessions.
9) Patients were aware of whether they received acupuncture or not. No mention was made of the level of awareness re: multiple groups.
10) Follow-ups were conducted at 3 and 12 months.
References: 1) http://www.strokeassociation.org : The web site of the American Stroke Association.
2) Bakheit, A. MD, et al. A Randomized, Double-Blind, Placebo-Controlled, Dose-Ranging Study to Compare the Efficacy and Safety of Three Doses of Botulinum Toxin Type A (Dysport) With Placebo in Upper Limb Spasticity After Stroke, Stroke. 2000;31:2402-2406.
3) Brashear, Allison M.D. Intramuscular injection of botulinum toxin for the treatment of wrist and finger spasticity after a stroke. N Engl J Med 2002 Aug 8;347(6):395-400
4) Brown, D.A. PhD, PT; S.A. Kautz, PhD. Increased Workload Enhances Force Output During Pedaling Exercise in Persons With Poststroke Hemiplegia. Stroke. 1998;29:598-606
5) Gelber, David A. MD et al, Open-Label Dose-Titration Safety and Efficacy Study of Tizanidine Hydrochloride in the Treatment of Spasticity Associated With Chronic Stroke. Stroke. 2001; 32: 1841-1846.
6) Gosman,-Hedstrom, et al. Effects of Acupuncture Treatment on Daily Life Activities and Quality of Life A Controlled, Prospective, and Randomized Study of Acute Stroke PatientsStroke. 1998; 29:2100-2108
7) Hesse, S. et al. Ankle Muscle Activity Before and After Botulinum Toxin Therapy for Lower Limb Extensor Spasticity in Chronic Hemiparetic Patients S. From the Klinik Berlin, Department of Neurological Rehabilitation, Free University Berlin (Germany) (S.H., D.L., M.T.J., K.H.M.), and the Rehabilitation Institute, Ljubljana, Slovenia (J.K., M.G.). Correspondence to Stefan Hesse, MD, Klinik Berlin, Kladower Damm 223, 14089 Berlin, Germany.
8) Hesse S, et al. Botulinum toxin treatment for lower limb extensor spasticity in chronic hemiparetic patients. J Neurol Neurosurg Psychiatry. 1994;57:1321- 1324.
9) Hu HH. A randomized controlled trial on the treatment for acute partial ischemic stroke with acupuncture., Neuroepidemiology. 1993; 12(2): 106-13.
10) Ivanhoe, MD, by Cindy B. Alberto Esquenazi, MD, and Nathaniel H. Mayer, MD. http://medbroadcast.healthology.com articles
11)Johansson, Barbro B. MD, Acupuncture and Transcutaneous Nerve Stimulation in Stroke Rehabilitation, Stroke. 2001; 32: 707-713.
12)Johansson, K RN, Sensory stimulation promotes normalization of postural control after stroke. Stroke 1994 Jun; 25(6): 1176-80.
13)Kjendahl A, A one-year follow-up study on the effects of acupuncture in the treatment of stroke patients in the sub-acute stage: a randomized, controlled study, Clin Rehabil. 1997 Aug; 11(3): 192-200.
14)McGuire JR, Harvey RL. The prevention and management of complications after stroke. Phys Med Rehabil Clin North Am. 1999;10:857– 874.
15)Maciocia, Giovanni. The Practice of Chinese Medicine, 1994, Churchill Livingstone.
16)Marieb, Elaine. Human Anatomy and Physiology, 4th Edition, 1998, Addison Wesley Longman
17)Meythaler, Jay M. Intrathecal Baclofen for Spastic Hypertonia From Stroke, Stroke. 2001;32:2099-2109
18)Nan, Fatma. Pathophysiology And Rehabilitation Of Upper And Lower Motor Neuron Syndromes, Hacettepe University.
19)Ogawa N, Asanuma M, Hirata H, Ota Z, Yamawaki Y, Yamamoto M. Development of a simple spasticity quantification method: effects of tizanidine on spasticity in patients with sequelae of cerebrovascular disease. J Int Med
20)� J Pei. The effect of electro-acupuncture on motor function recovery in patients with acute cerebral infarction: a randomly controlled trial. J Tradit Chin Med 2001 Dec;21(4):270-2
21)Simpson D, et al. Botulinum toxin type A in the treatment of upper extremity spasticity: a randomized double-blind placebo controlled trial. Neurology. 1996; 46:1306 –1310.
22)Simpson, David MD, Professor of Neurology, Mount Sinai School of Medicine, and Jean-Michel Gracies, MD, Mt. Sinai School of Medicine, as cited on www.poststrokehelp.com
23)Stamenova, P. A randomized, double blind, placebo-controlled study of the efficacy and safety of tolperisone in spasticity following cerebral stroke. European Journal of Neurology, 2005; 1 QA2 (6): 453-461).
24)Steultjens, Esther MA et al. Occupational Therapy for Stroke Patients. Stroke. 2003;34:676-687
25)Wallace JD. Summary of combined clinical analysis of controlled clinical trials with tizanidine. Neurology. 1994;44(suppl 9):S60 –S69.
26)Werner, C. et al. Treadmill training with partial body weight support and an electromechanical gait trainer for restoration of gait in sub-acute stroke patients. Stroke, 2002; 33:2895.
27)Weimar C, et al. Assessment of functioning and disability after ischemic stroke. Stroke. 2002;33:2053–2059.
28)Wiener, J et al. Measuring the Activities of Daily Living: Comparisons Across National Surveys, Journal of Gerontology: SOCIAL SCIENCES (November 1990, Volume 45, Number 6, pp.S229-237).
29)Wojner AW. Optimizing ischemic stroke outcomes: an interdisciplinary approach to post-stroke rehabilitation in acute care. Crit Care Nurs Q.
Sharon Rose, L.Ac. Acupuncture and Post-Stroke Spasticity 20 1996;19:47–61.
30)Wong, AM Clinical trial of electrical acupuncture on hemiplegic stroke patients. Am J Phys Med Rehabil 1999 Mar-Apr;78(2):117-22.
31)Wu, Yan. Practical therapeutics of Traditional Chinese Medicine, 1997, Paradigm Publications.
32)Young RR. Spasticity: a review. Neurology. 1994;44 (suppl 9):S12–S20.
33)Young RR. Physiologic and pharmacological approaches to spasticity. Neurol Clin. 1987; 5:529 –539.